Learn What's Up
Deceptive Sexuality & Trauma Resource Library
Education on how maintaining a secret sexual life is psychological abuse that causes trauma to intimate partners, relationships, children and families, and where theories of infidelity, sex addiction, and compulsive sexual behavior converge with treatments for systemic abuse, injustice and complex trauma into a plane of extraordinary space and vibrational science. And now, in 2026, this work enters its next phase —the emergence of Voice-Up Culture and an Alpha Masculinity grounded in honesty, accountability, and care.
Education on how maintaining a secret sexual life is psychological abuse that causes trauma to intimate partners, relationships, children and families, and where theories of infidelity, sex addiction, and compulsive sexual behavior converge with treatments for systemic abuse, injustice and complex trauma into a plane of extraordinary space and vibrational science.
DSTT Info
What is Deceptive Sexuality?
Couples and individuals dealing with problematic sexual behaviors might typically hear the terms compulsive sexual behavior disorder, sexual addiction, infidelity used to describe their experiences. But these words don’t fully capture the holistic nature of what actually goes on in these situations. An exclusive focus on sexual behaviors is incomplete, as problematic sexual behaviors are often accompanied by a tragic pattern of abuse and injury that deeply impacts partners and family members for years to come.
Deceptive Sexuality and Trauma (DST) presents a more complete picture of the presence and impact of sexual acting-out behaviors. Deceptive sexuality refers to problematic sexual behaviors in combination with associated patterns of domestic and intimate partner abuse that frequently leads to devastating traumatic injuries. In other words, deceptive sexuality is a clinical syndrome that involves two pathological systems: one that relates to the inability to control sexual urges or behaviors and/or sexual entitlement (which we call Compulsive-Entitled Sexuality, or CES), and another that includes integrity violations and abusive actions (Integrity-Abuse Disorder, or IAD).
Many people suffer from deceptive sexuality and experience significant psychological, social, and life consequences as a result. These individuals, along with their partners and family members, often seek professional treatment and need clinical support. Unfortunately, we lack a formal, professional consensus on how to best to diagnose and treat this issue.
What is a Deceptive, Compartmentalized, Sexual-Relational Reality, DCSR?
Deceptive sexuality involves someone having a deceptive, compartmentalized, sexual- relational reality in the context of an intimate relationship(s) or family system. Think of it as something like a Secret Sexual Basement – a place that houses a person’s deceptively hidden sexual, romantic, and/ or emotional intimacy with others that is not shared with the primary intimate partner. A place that is characterized by an ongoing system of psychological and relational control, domination, violation, and harm.
The majority of people who struggle with repetitive and problematic sexual behaviors and seek clinical intervention are in relationships (often intimate partnerships or marriages), have families, and may be parents as well. In fact, most clinicians working with these individuals indicate that one of the primary motivators for treatment is the impact on the partnership, the marriage, and/or the family.
What has not been part of the focus in any of the dominant diagnostic and treatment models is that patterns of repetitive and problematic sexual behaviors are often part of a deceptive, compartmentalized sexual or relational reality (DCSR) within the context of intimate relationship(s). DCSRs are intentionally hidden and separated from the rest of the person’s life and reality, which has a huge, negative impact on the person’s partner and family.
The educational metaphor of, “the secret sexual basement”, is synonymous with the clinical term, DCSR, which is a sexual or reality that is being covertly managed through a strategic psychological operation of intentionally manipulated reality (IMR) used by the abuser to keep two realties separate in attempt to prevent the people upstairs from knowing the truth of their realities. In fact, deceptive sexuality trauma (DST), can be described as the traumatic injuries and symptoms that occur from being subjected to a DCSR, deceptive, compartmentalized, sexual-relational reality.
What is the Educational Metaphor: The Secret Sexual Basement?
According to the DST Model, deceptive sexuality includes behaviors aimed at creating and maintaining a deceptive, compartmentalized, sexual reality (DCSR). The technical term DCSR is understood metaphorically through the concept of a secret sexual basement. The metaphor of a secret sexual basement helps us better identify and understand the integrity abuse. Through metaphor, we recognize that in addition to the sexual, relational behaviors occurring in the basement, there is also the process of creating the basement as well as the psychology and behavioral tactics that keep the basement in place. An ongoing, covert deceptive system takes places that manipulates reality and relational dynamics in an effort to sustain the basement, effectively harming and traumatizing everyone in the house.
Professionals who work with individuals impacted by deceptive sexuality must be aware of the multi- faceted factors involved in creating and maintaining secret sexual basements. Truly understanding this complicated system and addressing the integrity abuse involves treating more than just the behaviors in the basement. It also requires focus on the psychology and behaviors involved in the creation and maintenance of the DCSR.
What is Compulsive-Entitled Sexuality (CES)?
Compulsive-Entitled Sexuality (CES) refers to an inability or an unwillingness to control sexual urges or behaviors, even when they cause significant negative consequences. People may experience CES because of a compulsive-addiction disorder and/or a pathological level of perceived sexual entitlement. Indeed, many patients present with at least some behavioral control problems and sexual entitlement.
Examples of CES include a lack of ability to control impulses or a perceived sense of entitlement as well as engaging in problematic patterns of pornography use, infidelity, prostitution, cybersex, flirting. Sometimes CES can extend into clinical concerns such as sexual offending, abuse of power in the workplace, etc.
The Deceptive Sexuality and Trauma Model proposes that CES is one of the primary symptoms of the deceptive sexuality diagnosis. In addition to being a main driver of problematic sexual behavior patterns, CES also plays a big role in associated abusive behaviors such as lying, deception, and psychological manipulation.
What is Integrity-Abuse Disorder (IAD)?
- a long-term pattern of disregard for, or violation of, the rights of others
- a demonstrated lack of empathy toward others
- deception and manipulation of the truth
- psychological manipulation of others’ realities (gaslighting)
- exploiting others for personal gain or pleasure through
- superficial charm, seduction, or intimidation
- deficits in integrity, and/or morality
- impulsivity and reckless behaviors
- partner, relationship, child, and/or family risk-taking and endangerment
- a lack of remorse; callous attitude toward those people harmed
- intentional withholding of life-altering survival-based information
- externalizing of responsibility
- defensive tactics that violate integrity
- victim-blaming or relationship-blaming
- an ongoing system of covert domination/control and coercive control
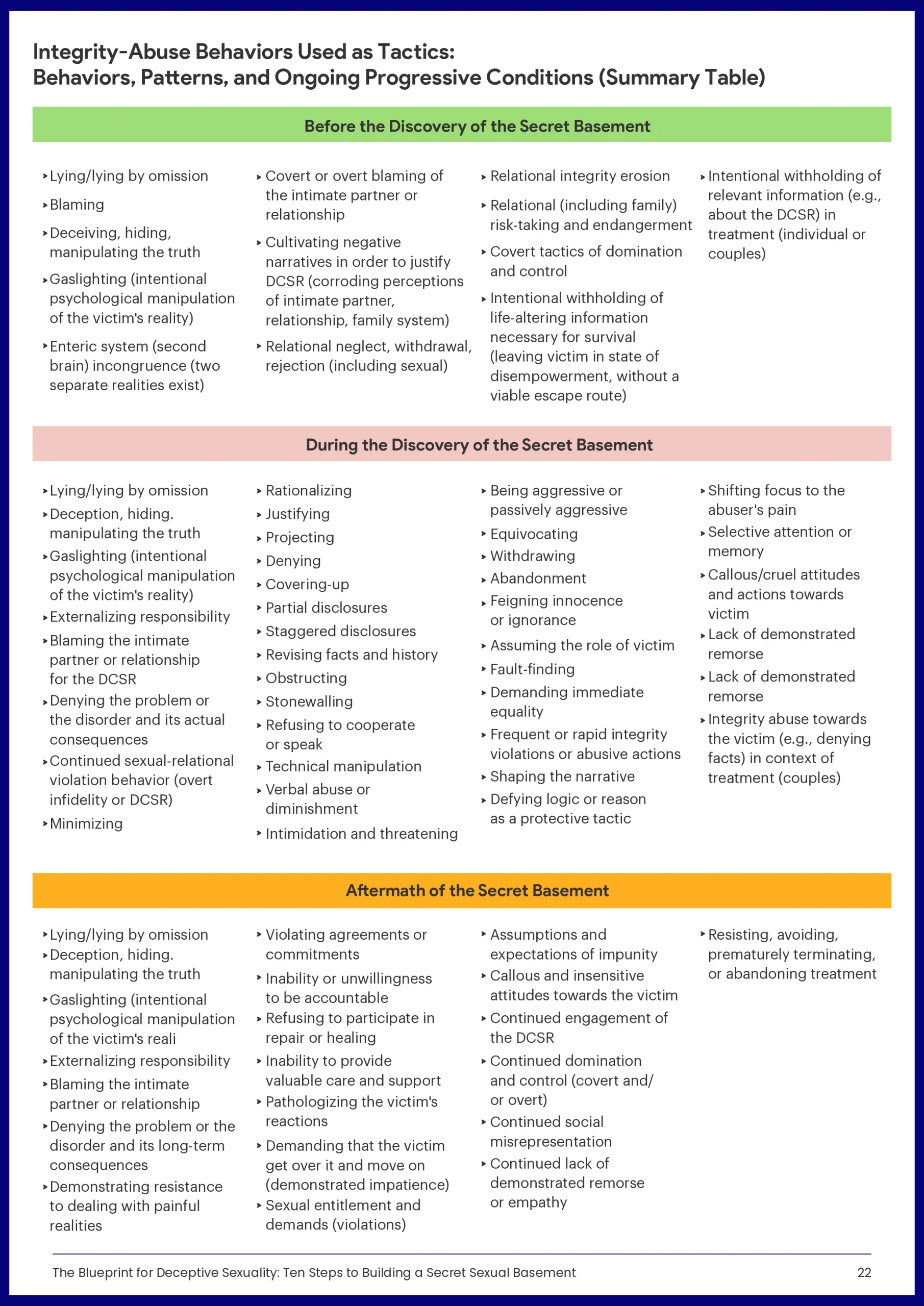
How is a Secret Sexual Life a System of Covert Dominance and Control?
During the covert phase, abusers tend to have a significant amount of covert power and control over their partners, including coercive control (a catch-all term that emphasizes the core of most domestic abuse, which is the need for power and control over another person and incorporates numerous types of nonphysical domestic abuse patterns; Candela, 2016). By withholding important information from their partners, they effectively strip away their partners’ ability to truly understand key aspects of their intimate relationships, along with the power to make healthy, self-protective decisions. Abusers who hold sexual secrets prevent their partners from taking action based on reality, and ultimately keep them paralyzed in a destructive pattern of uninformed immobility or chronic disempowerment and coercive control (Candela, 2016). There are some abusers who have convinced themselves that it is considerate and protective to intentionally keep their partners and family members unaware of the DCSR, as if it’s an act of chivalry. This belief reinforces a sense of power and dominance and assumes that the partner and family members are too weak to handle the DCSR, that they need protection from it, or that they are somehow not worthy of being able to determine their own destinies.
Why the Term Deceptive Sexuality Trauma?
The specific term, deceptive sexuality trauma, refers specifically to the trauma that results from prolonged subjugation, over time, to the specific type of sexual-relational integrity-abuse and compulsive-entitled sexuality behaviors and patterns that are often experienced by victims of deceptive sexuality. This trauma often includes CTS that results from integrity abuse in all three phases of the trauma: the covert, exposure, and symptom progression phases (essentially before, during, and after the discovery of the secret sexual basement). The CTS involves a slow and progressive shaping of the victim’s psychological systems over time: the self, relationship to the abuser, reality, the second brain system, relational integrity, and core functions related to identity (e.g., sexuality, gender, and body), attachment relationships, and systems of meaning.
DST is a term developed directly from victims of deceptive sexuality. It is highly specific and limited in scope compared to other types of traumas (which may be applied to many other injuries and contexts). For example, attachment injury or betrayal trauma may have nothing to do with deceptive sexuality at all. So, while deceptive sexuality includes many other traumas, it is distinct and is the trauma from DCSRs, different from betrayal trauma (Freyd, 2008) or attachment trauma science and theory (Johnson, S., 1996).
Deceptive sexuality trauma (DST) refers to both the traumatic injuries and the trauma symptoms experienced by intimate partner(s) and family members of people who engage in deceptive sexuality. Deceptive sexuality often involves the victimization of others through entitled sexuality and patterns of psychological, emotional, and relational abuse (or Integrity-Abuse-Disorder, IAD). Having been subjected to ongoing patterns of both Compulsive-Entitled Sexuality (CES) and Integrity Abuse (IA) over time, victims of deceptive sexuality often experience a specific type of trauma and stressor-related symptoms known as DST.
The Deceptive Sexuality Trauma (DST) Model proposes that CES and IAD cause individuals to behave in ways that are abusive, that prohibit partners from being able to respond in healthy ways based on being informed about their reality, and that lead to significant traumatic symptoms and injuries for partners and family members. According to this model, deceptive sexuality – and associated patterns of psychological deception and manipulation – represent a specific type of system of abuse that causes a specific type of trauma.
What is the Difference Between Betrayal Trauma and Deceptive Sexuality Trauma?
Deceptive sexuality trauma, or DST, must not be mistaken or misunderstood as meaning the same as the more general term, betrayal trauma. The science behind the term, betrayal trauma (Gómez, J. M. & Freyd, J. J., 2019), is distinct and different from the science of deceptive sexuality trauma (Minwalla, 2019), and hence is important that people know the differences so that they can be informed as they seek help and treatment.
Betrayal Trauma: Betrayal trauma (Gómez, J. M. & Freyd, J. J., 2019, Freyd, J. J. & Birrell, P. J., 2013, Freyd, J. J., 2008, Freyd, J. J., 1997, Freyd, J. J., 1996) occurs when the people or institutions on which a person depends for survival significantly violate that person’ s trust or well-being. Betrayal trauma can apply to many situations and types of harm and injury, and the academic science and literature on betrayal trauma includes focus on childhood physical, emotional, or sexual abuse perpetrated by a caregiver and institutional betrayal, as examples.
References:
Gómez, J. M. & Freyd, J. J. (2019). Betrayal trauma. In J. J. Ponzetti (ed.), Macmillan Encyclopedia of Intimate and Family Relationships: An Interdisciplinary Approach (pp. 79-82). Boston, MA: Cengage Learning Inc. https://dynamic.uoregon.edu/jjf/articles/gf2019.pdf
Freyd, J. J. & Birrell, P. J. (2013). Blind to Betrayal. John Wiley & Sons. https://sites.google.com/site/betrayalbook/
Goldsmith, R. E., Freyd, J. J., & DePrince, A. P. (2012). Betrayal trauma: Associations with psychological and physical symptoms in young adults. Journal of Interpersonal Violence, 27(3), 547–567. https://doi.org/10.1177/0886260511421672
Freyd, J. J. (2008) Betrayal trauma. In G. Reyes, J.D. Elhai, & J.D. Ford (eds.), Encyclopedia of Psychological Trauma. New York: John Wiley & Sons. https://dynamic.uoregon.edu/jjf/articles/freyd2008bt.pdf
Freyd, J. J. (1997). Violations of power, adaptive blindness and betrayal trauma theory. Feminism & Psychology, 7(1), 22–32. https://doi.org/10.1177/0959353597071004
Freyd, J. J. (1996). Betrayal Trauma: The Logic of Forgetting Childhood Abuse. Cambridge: Harvard University Press. https://www.tandfonline.com/doi/abs/10.1080/00029157.1998.10403432
Deceptive Sexuality Trauma (DST): Deceptive sexuality trauma (Minwalla, 2019, Minwalla, 2012) is a diagnostic term for a specified trauma-and stressor related disorder, which occurs when people are subjected to and victimized by ongoing patterns of Compulsive-Entitled Sexuality (CES) and Integrity-Abuse (IA) in the context of being in an intimate partnership or family system, which is diagnosed as a specified partner or spouse psychological abuse disorder, called deceptive sexuality (Minwalla, 2019).
- Deceptive sexuality trauma includes betrayal trauma but is not the same. Deceptive sexuality trauma describes the trauma that occurs from Deceptive, Compartmentalized, Sexual and/or Relational Realities (DCSR), basically the trauma from infidelity and having a secret sexual life, recognizing the psychological operation of Intentionally Manipulated Reality (IMR) and describing those traumatic injuries and symptoms that occur from that specific Integrity-Abuse-Disorder (IAD).
- Betrayal trauma is a more general term that may include childhood sexual abuse or institutional betrayal.
- Betrayal trauma theory (Freyd, J. J., 1997) does not describe the 22 traumatic injuries and symptoms based on deceptive sexuality and trauma grounded theory, which articulates the impact of deceptive, compartmentalized, sexual and relational reality in the context of an intimate relationship or family system, referred to as DST-22.
- Betrayal trauma theory (Freyd, J. J., 1997) does not name Compulsive-Entitled-Sexuality (CES), or Integrity-Abuse-Disorder (IAD), a specified psychological abuse disorder and form of intimate partner abuse and relationship maltreatment.
- Deceptive Sexuality and Trauma (DST) is a specified type of trauma that includes the impacts of compulsive sexual behavior disorder, sexual addiction, sexual and emotional infidelity, post-infidelity trauma, attachment trauma, psychological intimate partner and relationship abuse and trauma, attachment injury and trauma, betrayal trauma, institutional betrayal trauma, psychological abuse disorder, acute stress and post-traumatic stress, and complex trauma, and hence should not be reduced simply to “betrayal trauma”.
What is the Problem with Traditional Treatments for Infidelity and Sex Addiction?
Traditional clinical models for understanding sexual acting out problems have focused solely on the repeating sexual behaviors, while often ignoring the chronic sociopathic and abusive behavioral patterns, the psychological abuse disorder, and a specified intimate partner abuse. Essentially, these models have focused on only one part of a two-part problem. In doing so, they have neglected and omitted other significant problematic behaviors from clinical recognition and treatment.
Further, these models and practitioners do not view those who create and maintain Deceptive, Compartmentalized Sexual or Relational Realities (DCSRs) as experiencing a form of mental disorder or abuse problem. Instead, the focus of traditional approaches is on the diagnosis of the sexual behaviors (compulsive or addictive), the lack of sexual control, the cause of the sexual behavior patterns, and the negative consequences experienced by the person who is sexually acting out. The primary problems with these models include:
- Failure to recognize the abuse. The first problem with traditional clinical models is that they don’t acknowledge the patterns of emotional, psychological, and relational abuse perpetrated on intimate partners and families of those with deceptive sexuality. Deceptive sexuality is indeed a particularly destructive form of intimate partner abuse and domestic abuse. Often, there are ongoing patterns of abuse that victims experience for years, and the consequences are significant. This type of abuse is psychological in nature, not physical. It is the covert psychological operation required to keep two realities separate, the upstairs of the metaphorical house, and the secret sexual basement downstairs, being kept separate through intentionally manipulating the reality (IMR) of the people upstairs. It is a psychological operation, that just like similar military operations, are designed to weaken and gain power over people, and hence a form of covert domination and control.
- Failure to recognize the trauma. Traditional clinical models do not recognize or understand the trauma symptoms experienced by these partners and family members. Sadly, however, this type of trauma is pervasive, intensely distressing, and in need of timely and appropriate diagnosis and treatment. Traditional models have ignored these trauma-related symptoms, and few practitioners in the psychological field as a whole have a solid conceptualization of this type of trauma. Deceptive sexuality trauma, or DST, is a specified trauma-and stressor related disorder, which occurs when victims are subjected to ongoing patterns of Compulsive-Entitled Sexuality (CES) and Integrity-Abuse (IA) in the context of an intimate partnership or family system, which is diagnosed as a specified partner or spouse psychological abuse disorder, called deceptive sexuality. DSTT has identified and describes 22 traumatic injuries and symptoms based on grounded theory referred to as the DST-22, which informs clinical assessment, stabilization, and treatment for survivors.
- Failure to recognize and support the victims. In addition to not recognizing the trauma, many clinical models lack consciousness about the victims of deceptive sexuality. There has been a profound neglect of the partners and families who are exposed to, and impacted by, these problems. Traditional treatment models have either excluded partners and family members from clinical consideration or, even more damaging, have tended to misdiagnose them. Some models rely on general couples or sex therapy approaches, while others still use victim-blaming interventions based on the traditional concepts of co-sex addiction and codependency. Partners are often “educated” that their responses and reactions are actually part of the relationship problem or are symptoms of a co-addiction that require treatment and management. Unfortunately, none of these approaches appropriately recognize, diagnose, or attempt to treat the abuse, victimization, and specified trauma-related symptoms.
- Failure to identify a disorder. The field frequently uses terms such as sex addiction, compulsive sexual behavior, out of control sexual behavior, and impulse control problem, or infidelity. But these terms do not attempt to describe any type of abuse problem, sociopathic behavior patterns, or conduct disorder. The field has clearly failed to recognize the presence and impact of deceptive sexuality as a type of disorder. There is no established awareness of an integrity-abuse disorder as the cause of the abuse/trauma. And there are no notable efforts put towards recognizing the role of a systemic abuse problem in causing significant trauma-related symptoms.
Unfortunately, abuse and trauma caused by deceptive sexuality are buried in the shadows of normalization, denial, and our collective lack of insight.
This needs to change.
Abuse and trauma caused by deceptive sexuality must be researched and more deeply understood by psychological practitioners and clinical researchers. We must better understand so that we can develop effective diagnostic and treatment approaches that address both sexual behaviors and abuse patterns that result in experiences of short- and long-term trauma.
What is the Deceptive Sexuality and Trauma (DST) Model?
The Deceptive Sexuality and Trauma (DST) Model expands the understanding, diagnosis, and treatment of sexual acting out disorders. It identifies deceptive sexuality as a form of domestic abuse. It represents a clinical step forward in the field and a significant advancement in the treatment of sexual acting out. This model confronts the traditional and current models of treatment and brings a critical set of new arguments to the ongoing debate related to sex addiction, compulsive sexual behaviors, and infidelity. This new clinical paradigm is organized around three foundational clinical concepts: Compulsive-Entitled-Sexuality (CES); Integrity-Abuse-Disorder (IAD), and a resulting specified type of trauma among victims (Deceptive Sexuality Trauma).
The DST Model revises the clinical paradigm of sexual acting-out behaviors in at least three important ways:
- The DST Model expands the traditional, single-concept diagnosis of either sex addiction or compulsive sexual behavior to include Compulsive-Entitled- Sexuality (CES), recognizing the role of sexual entitlement as a major factor that contributes to problematic sexual behavior patterns.
- The DST Model gives attention to the roles that conduct disorder and covert psychological and relational abuse behaviors play in sexual acting-out behaviors and considers these pathological patterns to be a type of Integrity-Abuse-Disorder (IAD).
- The DST Model identifies partners and family members of people with Deceptive Sexuality as victims of abuse who often experience devastating trauma symptoms. As such, this model shines a light on the abuse-victim dynamic that so frequently occurs in these situations and challenges the codependency view that has often been associated with the single-concept diagnosis of co-sex addiction.
The DST Model proposes that Compulsive-Entitled-Sexuality (CES) and Integrity-Abuse-Disorder (IAD) cause individuals to sexually act out in ways that lead to significant traumatic injuries for their victims. Importantly, the model recognizes that in such situations, abuse problems exist in addition to sexuality issues. Further, this model replaces existing victim-blaming models with abuse-trauma awareness and treatment approaches.
Why Deceptive Sexuality and Trauma Treatment?
DSTT addresses the psychological abuse called integrity abuse, which is a psychological operation of Intentionally Manipulated Reality (IMR). DSTT addresses this missing piece. DSTT subsumes traditional models for infidelity, sex addiction and compulsive sexual behavior disorder, in that it:
- Remedies the victim-blaming and diagnostic mislabeling of deceptive sexuality victims
- Designates a name for the abuse disorder associated with deceptive sexuality
- Provides effective treatments for abusers, victims, and the relationships injured by deceptive sexuality
- Helps mental health professionals recognize and treat the abusive impacts of deceptive sexuality from an abuse-victim-trauma consciousness
Abuse-Victim-Trauma (AVT) Consciousness?
DSTT applies an abuse-victim-trauma consciousness to the diagnosis and clinical treatment and management of compulsive sexual behavior disorder, sex addiction, and infidelities. The model focuses on the process of perceiving, identifying, recognizing, naming, changing, and evolving our understanding of abuse, the victimization of human beings, and the resulting traumatic impacts. Abuse-victim-trauma consciousness is essential for understanding deceptive sexuality and is the primary contribution of the DSTT clinical model. Treatment for deceptive sexuality should be informed by a consciousness of an abuse dynamic; an abuser, victim(s), and abusive-injured relationship(s). Treatment should not be solely focused on a sexuality problem or a moral problem.
What is the Minwalla Model?
The Minwalla Model refers to Dr. Minwalla’s emerging consciousness; his set of teachings, evolving concepts, and voice, intended to illuminate abuse-victim-trauma-existing realities, human sexuality, gender, masculinity, and human rights in order to move humanity towards justice. This includes the articulation of a conscious technology and practice of creating extraordinary space for the purposes of learning and healing- a modality based on Intentional Vibe Theory (IVT). DSTT is simply Dr. Minwalla’s current focal point of illumination, the vanishing point of infidelity and sex addiction treatment, a derivative of the broader Minwalla Model, which exists as an expansive dimensional plane of perspective and consciousness.
What is Intentional Vibe Theory (IVT)?
Intentional Vibe Theory (IVT) postulates that Intentionally Manipulated Reality (IMR) promotes disease and that Intentionally Accurate-Authentic Reality (IAR) promotes health and informs Intentional Vibe Theory Treatment (IVTT), a psychological healing model, method and vibrational science that defines a unique treatment for trauma, particularly systemic abuse and injustice, and the complex trauma sequences that result to not only individuals but groups of peoples and communities. IVTT based approaches usher in a unique method and way of treating systemic abuse and complex trauma disorders, intended to help humanity move towards justice and psychological health.
Terms
Deceptive Sexuality (DS):
Deceptive Sexuality (DS) involves someone having a deceptive, compartmentalized, sexual- relational reality in the context of an intimate relationship(s) or family system, and is diagnosed by two interrelated psychological disorders, Compulsive-Entitled Sexuality (CES) and Integrity-Abuse-Disorder (IAD), a specified psychological abuse disorder and form of intimate partner abuse and relationship maltreatment. Deceptive Sexuality (DS) is a clinical syndrome that involves two pathological systems: one that relates to the inability to control sexual urges or behaviors and/or sexual entitlement (which we call Compulsive-Entitled-Sexuality, or CES), and another that includes integrity violations and abusive actions (Integrity-Abuse-Disorder, or IAD). (Minwalla, 2018)
Deceptive Sexuality Trauma (DST):
Deceptive Sexuality Trauma is the clinical diagnostic term for the specified trauma-and stressor related disorder, which occurs when people are subjected to, and victimized by, ongoing patterns of Compulsive-Entitled Sexuality (CES) and integrity-abuse while in the context of an intimate partnership and/or family system. DST the specified trauma caused by deceptive sexuality, which is a specified psychological abuse disorder.
Compulsive Sexuality (CS):
Sexual behavior where the person lacks control or is not able to stop or resist engaging despite negative consequences signifying a potential impulse control or addiction-based problem.
Sexual Entitlement (SE):
An unhealthy psychology of the prioritization of personal sexual experience and gratification over the human rights of, and harmful impacts on others.
Compulsive-Entitled Sexuality (CES):
Compulsive-Entitled Sexuality is the inability to control sexual behaviors in combination with a psychology of sexual entitlement, and specifically refers to an inability and/or an unwillingness to control sexual urges or behaviors, even when they cause significant negative consequences. (Minwalla, 2018)
Integrity Disorder:
An endogenous problem characterized by deficits in integrity and the inability to be honest or truthful. (Minwalla, 2018)
Integrity Abuse (IA):
Integrity violations and intentionally manipulative abusive actions and patterns that cause harm or injury to other people and relationships and result from a lack of integrity. (Minwalla, 2018)
Integrity-Abuse Disorder (IAD):
A type of conduct disorder, a specified psychological abuse disorder, defined by a significant lack of integrity and a (covert) relational abuse system of domination and control. Integrity violations and abusive actions that result from deficits in integrity cause harm or injury to other people and relationships and cause significant impairment to important areas of life functioning. (Minwalla, 2018)
Deceptive, Compartmentalized, Sexual- Relational Reality (DCSR):
A person’s deceptively hidden sexual, romantic, and/or emotional intimacy with others that is not shared with the primary intimate partner. DCSRs are intentionally hidden and separated from the rest of the person’s life and reality, relying on the psychological operation of intentionally manipulated reality (IMR). (Minwalla, 2018)
Deceptive:
Tending or having power to cause someone to accept as true or valid what is false or invalid; perceptually misleading.
Compartmentalization:
A defense mechanism in which people mentally separate conflicting thoughts, emotions, or experiences to avoid the discomfort of contradiction; can also be a neutral term to simply refer to separating from the whole, to make a separate compartment.
Deceptive Compartmentalization (DC):
A type of integrity problem that involves separating something from the whole, deceptively, which by definition lacks integrity and is dishonest.
Sexual-Relational:
Refers to what is being deceptively compartmentalized, which is a reality consisting specifically of sexuality, emotional, romantic, and/or relational infidelity. The S and the R in the DCSR acronym refers to sexual-relational; the secret basement is specifically sexual-relational in nature.
Reality:
The world or the state of things as they exist, as opposed to an idealistic or notional idea of them, and the R in DCSR also refers to the word, Reality.
Secret Sexual Basement:
A metaphor for a DCSR; the terms can be used interchangeably with the educational metaphor, the Secret Sexual Basement refers to a secret sexual or relational life, represented by the metaphor of a basement secretly built by a family member or one partner. It represents a person’s deceptively hidden sexual, romantic, and/or emotional intimacy with others that is not shared with the primary intimate partner, like having a secret sexual-relational basement that the person built underneath the relationship or family home. (Minwalla, 2021)
Pre-Existing Reality-Ego (PRE):
Everything that the partners and family members thought was real about their lives prior to discovering or becoming aware of the DCSR’s existence.
Complex Trauma:
Complex trauma is defined as repeated patterns of harm, with a consistent theme, that occur over a prolonged period, in which the victim lacks a viable escape route or is disempowered. (Herman, 1997)
Complex Trauma Shaping (CTS):
Complex Trauma Shaping (CTS) involves patterns of harm that exist over a period of time and in the context of disempowerment or the lack of a viable escape route. These experiences shape a person’s psyche over time, like drops of water on a rock (Minwalla, 2015). CTS is a process that gradually develops in response to the long-term progressive patterns of psychological, emotional, and relational harm.
Betrayal Trauma:
Is any abuse or violation that occurs within a close relationship of trust, and refers to a social dimension of psychological trauma, independent of post-traumatic stress reactions (Freyd, J., 1996). Childhood physical, emotional, or sexual abuse perpetrated by a caregiver are examples of betrayal trauma (Freyd, J., 2008).
Post-Infidelity Trauma:
Post-Infidelity Trauma refers to stress reactions and trauma-related symptoms that result from discovering infidelity in an intimate relationship.
Post-Traumatic Stress:
Post-Traumatic Stress involves a single or distinct event or traumatic incident, which results in symptoms of intrusions, avoidance or constrictions, and hyperarousal. Many partners and family members of those who engage in deceptive sexuality develop symptoms that meet most of the criteria for post-traumatic stress-related symptoms, including:
- Exposure to extreme stress intrusive re-experiencing of integrity-abuse or traumatic incidents
- Frequent episodes of triggering and reactivity
- Hyperarousal and hypervigilance
- Persistent avoidance or numbing
- Negative alterations in both thoughts and mood
- Anxiety about potential disease and contamination
- Worries about child safety, family, social repercussions
- Social isolation
- Significant embarrassment and shame
- Intense relational rupture and attachment injuries
- Gender, sexuality, and body alterations
Attachment Injury and Trauma:
An attachment injury is characterized by an abandonment or by a betrayal of trust during a critical moment of need (Johnson, S., 1996). Attachment injuries can act as traumatic events, which then cause post-traumatic stress symptoms and/or insecure attachments and relationship templates.
Intimate Partner Abuse and Trauma:
Intimate partner abuse and relationship violence, which includes psychological abuse, is known to cause fear and trauma, including post-traumatic stress and complex trauma. It also results in other negative mental health outcomes as well as impairment to life such physical health and economic functioning. (APA, 2013)
Coercive Control:
A catch-all term that emphasizes the core of most domestic abuse, which is the need for power and control over another person and incorporates numerous types of nonphysical domestic abuse patterns (Candela, 2016).
Psychological Abuse:
A form of abuse characterized by a person subjecting or exposing another person to behavior that may result in psychological trauma, including post-traumatic stress. It is often associated with situations of power imbalance in abusive relationships, where one person maintains control and power over the victim and engages in behaviors such as bullying, gaslighting, or child abuse.
Spouse or Partner Abuse, Psychological:
Is considered in the American Psychiatric Association: Diagnostic and Statistical Manual of Mental Disorders (DSM-V) under other conditions that may be a focus of clinical attention. Code 995.82 (T74.31XD) is the designation for the abuser, and Code V61.1 (Z69.11) is the designation used for encounter for mental health services for victim of spouse or partner psychological abuse (APA, 2013, p.721).
Other-Specified Trauma-and Stressor-Related Disorder:
Is considered in the American Psychiatric Association: Diagnostic and Statistical Manual of Mental Disorders (DSM-V) as a diagnosis, under Trauma-and Stressor- Related Disorders. “This category applies to presentations in which symptoms characteristic of a trauma-and stressor-related disorder that cause clinically significant distress or impairment in social, occupational, or other important areas of functioning predominate but do not meet the full criteria for any of the disorders.” (American Psychiatric Association, 2013, p. 289). The American Psychiatric Association further notes that a specific reason (e.g., Deceptive Sexuality Trauma, or DST) should be noted after the diagnosis of other specified trauma-and-stressor-related disorder.
Gender-Based Violence (GBV):
Refers to harmful acts directed at an individual based on their gender. It is often rooted in gender inequality and the abuse of power and harmful norms. GBV is a serious violation of human rights and a life-threatening health issue globally.
Acronyms
| FYI | For Your Information |
| ADT | Assess, Diagnose, Treatment Plan |
| ATC | Approach, Transition, Condition(s) |
| AVT | Abuse-Victim-Trauma |
| AVT-ER | Abuse-Victim-Trauma-Existing Reality(ies) |
| CES | Compulsive-Entitled Sexuality |
| CDC | Conscious Dignifying Circle/Clinic |
| C-PTSD | Complex Posttraumatic Stress Disorder |
| CSB | Compulsive Sexual Behavior |
| CTS | Complex Trauma Shaping |
| DCSR | Deceptive, Compartmentalized, Sexual-Relational Reality |
| DS | Deceptive Sexuality |
| DST | Deceptive Sexuality and Trauma (Model) |
| DST | Deceptive Sexuality Trauma (Symptoms) |
| DST-22 | The 22 Grounded Theory Traumatic Injuries and Symptoms of DST |
| GBT | Gender-based Trauma |
| GBV | Gender-based Violence |
| GP | Gender Pathology |
| IA | Integrity-Abuse |
| IAD | Integrity-Abuse Disorder |
| IAR | Intentionally Accurate-Authentic Reality |
| ICF | Intentional Clinical Frequency |
| IMR | Intentionally Manipulated Reality |
| ISH | Integrity, Safety, Humility |
| ISH | The Institute for Sexual Health, a Psychology Corporation, Inc. |
| IVT | Intentional Vibe Theory |
| IVTT | Intentional Vibe Trauma Treatment |
| PRE | Pre-Existing Reality-Ego |
| PTSD | Posttraumatic Stress Disorder |
| REF | Reality-Ego Fragmentation |
| RIT | Relational Integrity Theory |
FYI
DSTT Informational Justice Clarification Statement, Dr. Omar Minwalla, 2023
This clarification is to help people better understand how Deceptive Sexuality and Trauma Treatment (DSTT) is not the same as current treatments for infidelity, compulsive sexual behavior, or sex addiction. DSTT subsumes traditional treatment approaches and expands the field by illuminating blind spots, clinical errors, missing pieces, and ethical deficits in these current psychological treatments.
Deceptive Sexuality and Trauma Treatment (DSTT) is:
- Not a co-responsibility for infidelity model of treatment.
- Not a single diagnosis of compulsive sexual behavior disorder.
- Not the sex addiction model (i.e., it is not a single-diagnosis addiction concept only).
- Not a betrayal trauma treatment, betrayal recovery, or a partners of sex addicts trauma model. Deceptive sexuality trauma (DST) is different and distinct from betrayal trauma.
- Not a model that endorses, but refutes the concepts of co-sex addiction, prodependence/ prodependency, and/or codependency to treat survivors of psychological abuse or the abusive-injured relationship.
- Not a model that endorses, but refutes the concepts and the proposed treatments for sexual anorexia and/or intimacy anorexia.
- Not a model that endorses, but refutes the application of the Karpman drama triangle to victims of psychological abuse or to abusive-injured relationship(s).
- Not a problem sexuality diagnosis, and refutes attempts to modify human sexual arousal or to medicalize faith-based ideologies or misinformed moral judgment.
- Not a model that endorses, but refutes attachment-based treatments for intimate partner abuse, and instead utilizes a restorative justice model to treat abusive-injured relationship(s).
- Not a model that avoids the treatment of abuse, victimization, or trauma according to psychological practice guidelines and ethical responsibilities articulated clearly by the American Psychological Association (APA).
Dr. Minwalla’s voice, teachings, and grounded theory, Deceptive Sexuality and Trauma Treatment (DSTT), are explicitly not the same as any of the above. Instead, DSTT may subsume, or encompass as a subordinate some parts of these models, as is relevant for advancing the assessment, diagnosis, and treatment of infidelity, compulsive sexual behavior disorder, and sex addiction.
Important Note: Dr. Minwalla and DSTT support the health-promoting functions and conditions found by many men, and any person, in twelve-step programs, including important human vulnerability, voices, and fellowship. While DSTT does not rely or depend on recovery-based spiritual programming, DSTT does not oppose, but honors patient self-determination.
A Statement on Ethical Transparency in the Treatment of Infidelity & Sex Addiction:
A Statement to the Professional Community and the Public Regarding Psychological Treatment for Sex Addiction, Infidelity, and Partner Trauma
By Dr. Omar Minwalla
Alpha Shepherd, Mad Dad, the Triadic Core Whisperer
December 16, 2025
To my professional colleagues, treatment organizations, and to the public seeking psychological care,
I am speaking today in service of patients, ethical clarity, and professional integrity— particularly in the treatment of sex addiction, infidelity, and deceptive sexuality. For decades, individuals and families impacted by sex addiction have turned to clinicians, treatment centers, and professional organizations in good faith. They have entrusted us with their psychological safety, their financial resources, and their most intimate realities. With that trust comes a profound ethical responsibility: to be honest about what we diagnose, what we treat, and how we do so.
- Patients are not passive recipients of care.
- They are consumers of professional psychological services, and they are entitled to transparency.
What Patients Are Entitled to Ask
Any professional or organization offering treatment for sex addiction should be able to answer, clearly and publicly:
- What is your organizational history in treating the partners of sex addicts?
- When did you begin treating partners as patients in their own right?
- What treatment models have you used over time for partners of sex addicts?
- When exactly did those models change, what specifically changed, and why?
- What do you currently assess, diagnose, and treat in partners of sex addicts?
- Who provides that treatment—and with what licensure, supervision, and training?
- These are not hostile or political questions.
- They are basic informed-consent questions.
A Necessary Ethical Reckoning in the Sex Addiction Field
For many years, the sex addiction treatment field relied on the co-sex addict model. Under this framework, partners—overwhelmingly women—were routinely pathologized. Trauma responses to systemic gaslighting, chronic lying, prolonged subjugation to integrity-abuse, coercive control, and intimate partner abuse were misdiagnosed as co-sex addiction, codependency, or personality pathology, including borderline or histrionic.
This was not a minor theoretical disagreement.
It was a clinical mistake, a form and example of gender-based diagnostic mislabeling of patients seeking treatment for sex addiction, and a profound clinical and diagnostic failure that harmed thousands of patients across decades.
The American Psychological Association (APA) has long warned against the misdiagnosis of trauma in women, particularly when trauma symptoms are reframed as character or relational pathology. Yet, despite this guidance, there has been no meaningful public reckoning within the sex addiction field—no clear responsibility-taking, no apology to the partners harmed, and no transparent accounting of how or why these models were abandoned.
- Silence does not correct harm.
- Avoidance does not repair it.
Integrity-Abuse Must Be Explicitly Addressed in Sex Addiction Treatment
For over a decade, I have taught that sex addiction is not only a compulsive sexual behavior issue—it is also an integrity-abuse and psychological abuse issue. Chronic deception, gaslighting, and double-life behaviors constitute a form of intimate-partner abuse that must be named and treated as such.
As a result, professionals and organizations offering sex addiction treatment must now answer plainly:
- Do you assess sex addicts for integrity-abuse?
- Do you diagnose integrity-abuse when it is present?
- Do you treat the partner of a sex addict as a victim of psychological abuse?
- Is this diagnosis documented in treatment plans?
- If you do not treat integrity-abuse, do you clearly disclose that to patients?
- If you do, what is your treatment model, and what is it called?
- Ambiguity here is not neutral.
- It protects systems while leaving patients confused and vulnerable.
A Call for Transparency and Repair
Large sex addiction treatment organizations, residential treatment, and professional bodies have generated substantial revenue over decades while operating under evolving— or unclear—models of care. With that influence comes responsibility. The public deserves transparent answers to three simple questions:
- What is your organizational history in treating partners of sex addicts?
- What exact treatment model do you offer today?
- Whose clinical work and intellectual labor developed that model?
- This is not about blame.
- It is about truth, accountability, and ethical repair.
Why I Am Speaking Now
Purpose of This Statement
This statement is not intended to assign blame, allege misconduct, or characterize the motives of any individual or organization. Rather, it is an invitation to continued professional dialogue, ethical clarity, and alignment with best practices in integrity-abuse-trauma-informed care.
For many years, I have focused my efforts on education, clinical development, and patient advocacy within this field. I offer this statement in that same spirit: to encourage transparency, informed consent, and thoughtful reflection in the treatment of sex addiction, infidelity, and compulsive-impulsive sexual behavior disorder fields.
It is my professional position that patients affected by sex addiction—and the partners, children, and families who are often profoundly impacted—deserve clear information, accurate diagnosis, and the highest standards of ethical psychological care.
For many years, I chose restraint and silence in order to protect patients and support the evolution of the field. But silence, when it allows ongoing confusion or ethical evasion, becomes a form of participation.
I am speaking now, because partners of sex addicts deserve informed consent. Because truth matters in treatment.
And because integrity must be modeled—not merely taught.
It is now 2026. We should be able to clearly and honestly articulate what we offer to patients impacted by sex addiction.
Anything less fails the people who trusted us most.
With clarity and resolve,
Dr. Omar Minwalla
(MD = Mad Dad)
Licensed Psychologist & Clinical Sexologist
Founder, Institute for Sexual Health (ISH)
Originator, Deceptive Sexuality & Trauma Treatment Model
To my professional colleagues, treatment organizations, and to the public seeking psychological care,
I am speaking today in service of patients, ethical clarity, and professional integrity— particularly in the treatment of sex addiction, infidelity, and deceptive sexuality. For decades, individuals and families impacted by sex addiction have turned to clinicians, treatment centers, and professional organizations in good faith. They have entrusted us with their psychological safety, their financial resources, and their most intimate realities. With that trust comes a profound ethical responsibility: to be honest about what we diagnose, what we treat, and how we do so.
- Patients are not passive recipients of care.
- They are consumers of professional psychological services, and they are entitled to transparency.
What Patients Are Entitled to Ask
Any professional or organization offering treatment for sex addiction should be able to answer, clearly and publicly:
- What is your organizational history in treating the partners of sex addicts?
- When did you begin treating partners as patients in their own right?
- What treatment models have you used over time for partners of sex addicts?
- When exactly did those models change, what specifically changed, and why?
- What do you currently assess, diagnose, and treat in partners of sex addicts?
- Who provides that treatment—and with what licensure, supervision, and training?
- These are not hostile or political questions.
- They are basic informed-consent questions.
A Necessary Ethical Reckoning in the Sex Addiction Field
For many years, the sex addiction treatment field relied on the co-sex addict model. Under this framework, partners—overwhelmingly women—were routinely pathologized. Trauma responses to systemic gaslighting, chronic lying, prolonged subjugation to integrity-abuse, coercive control, and intimate partner abuse were misdiagnosed as co-sex addiction, codependency, or personality pathology, including borderline or histrionic.
This was not a minor theoretical disagreement.
It was a clinical mistake, a form and example of gender-based diagnostic mislabeling of patients seeking treatment for sex addiction, and a profound clinical and diagnostic failure that harmed thousands of patients across decades.
The American Psychological Association (APA) has long warned against the misdiagnosis of trauma in women, particularly when trauma symptoms are reframed as character or relational pathology. Yet, despite this guidance, there has been no meaningful public reckoning within the sex addiction field—no clear responsibility-taking, no apology to the partners harmed, and no transparent accounting of how or why these models were abandoned.
- Silence does not correct harm.
- Avoidance does not repair it.
Integrity-Abuse Must Be Explicitly Addressed in Sex Addiction Treatment
For over a decade, I have taught that sex addiction is not only a compulsive sexual behavior issue—it is also an integrity-abuse and psychological abuse issue. Chronic deception, gaslighting, and double-life behaviors constitute a form of intimate-partner abuse that must be named and treated as such.
As a result, professionals and organizations offering sex addiction treatment must now answer plainly:
- Do you assess sex addicts for integrity-abuse?
- Do you diagnose integrity-abuse when it is present?
- Do you treat the partner of a sex addict as a victim of psychological abuse?
- Is this diagnosis documented in treatment plans?
- If you do not treat integrity-abuse, do you clearly disclose that to patients?
- If you do, what is your treatment model, and what is it called?
Ambiguity here is not neutral.
It protects systems while leaving patients confused and vulnerable.
A Call for Transparency and Repair
Large sex addiction treatment organizations, residential treatment, and professional bodies have generated substantial revenue over decades while operating under evolving— or unclear—models of care. With that influence comes responsibility. The public deserves transparent answers to three simple questions:
- What is your organizational history in treating partners of sex addicts?
- What exact treatment model do you offer today?
- Whose clinical work and intellectual labor developed that model?
- This is not about blame.
- It is about truth, accountability, and ethical repair.
Why I Am Speaking Now
Purpose of This Statement
This statement is not intended to assign blame, allege misconduct, or characterize the motives of any individual or organization. Rather, it is an invitation to continued professional dialogue, ethical clarity, and alignment with best practices in integrity-abuse-trauma-informed care.
For many years, I have focused my efforts on education, clinical development, and patient advocacy within this field. I offer this statement in that same spirit: to encourage transparency, informed consent, and thoughtful reflection in the treatment of sex addiction, infidelity, and compulsive-impulsive sexual behavior disorder fields.
It is my professional position that patients affected by sex addiction—and the partners, children, and families who are often profoundly impacted—deserve clear information, accurate diagnosis, and the highest standards of ethical psychological care.
For many years, I chose restraint and silence in order to protect patients and support the evolution of the field. But silence, when it allows ongoing confusion or ethical evasion, becomes a form of participation.
I am speaking now, because partners of sex addicts deserve informed consent. Because truth matters in treatment.
And because integrity must be modeled—not merely taught.
It is now 2026. We should be able to clearly and honestly articulate what we offer to patients impacted by sex addiction.
Anything less fails the people who trusted us most.
With clarity and resolve,
Dr. Omar Minwalla
(MD = Mad Dad)
Licensed Psychologist & Clinical Sexologist
Founder, Institute for Sexual Health (ISH)
Originator, Deceptive Sexuality & Trauma Treatment Model

The following article was published in The National Psychologist in March 2015 and is preserved here in its original form, as The National Psychologist version is no longer available online. Original terms and acronyms are preserved to provide accurate historical context to the reader as to how the model was developed and has evolved:
‘Sexual Sobriety’ Leaves Victims Untreated
By Dr. Omar Minwalla, Psy.D.
March, 2015
The focus of traditional sex addiction-compulsivity treatment models tends to be diagnosing and stopping specific sexual behaviors, termed “sexual sobriety.” From a treatment perspective, it is correct and necessary to implement behavioral containment and stop destructive or problematic behaviors.
However, this is where most treatment ends, rather than also treating the other patterns of abuse of human beings and violations of human rights, termed “sex addiction-induced perpetrations” (SAIP).
The problem is sexual acting out disorders are not just sexual behaviors but are also abusive conduct patterns and complex pathologic systems, which often include elaborate deceptive compartmentalized sexual-relational realities and systems of abusive covert management.
These are patterns of methodical planning over time, careful construction of manipulation of others, and cognitive schemas well maintained to keep a compartmentalized reality protected from discovery. It takes pre-planning to sexually act out in many instances, sometimes requiring days of strategizing against the integrity of vital relational stability and family infrastructure required for health.
Maintaining a compartmentalized sexual or relational reality within a family system and relational intimate life takes profound energy to orchestrate, requiring careful and skilled methodology. This is not simply impulsive or compulsive sexual behavior.
A disorder of chronic lying in a family system is pathology and requires treatment, regardless of sexual acting out or not. Chronic patterns of establishing and maintaining a deceptive, compartmentalized sexual-relational system in an intimate relationship or family system is pathology and harmful, which is more accurate in description then simply “compulsive pornography use.”
The process of gaslighting an intimate partner – the intentional psychological manipulation of victim’s reality over time – is a form of emotional and psychological abuse and torture, eroding and damaging the victim’s survival instincts and intuition, regardless of sexual behaviors. Clearly, there exist many symptoms of pathology beyond the single symptom of “lack of control of specific sexual behaviors” or “compulsivity.” Sexual sobriety alone is an inadequate treatment model.
Sex addiction-induced perpetration (SAIP) is clinical pathology. However, within traditional treatment models there exists no established diagnostic or clinical formulation for SAIP and no treatment, methodology, or clinical paradigm that accounts for and treats SAIP. This is a serious omission in the field and in clinical practice.
The reality here is that the preoccupation with diagnosing and treating these complex pathologies as simply “compulsive” or impulse control disorders, and focusing on treating sexual behaviors, while avoiding and omitting the proper diagnosis of abuse and covert violence, leaves dynamics of serious pathology untreated.
This also means that the people harmed, the victims of these dynamics of abuse, are rendered invisible. Their trauma and experiences are not being accounted for in clinical treatment models and their suffering is being dishonored by the complete omission, silence and denial that pervade existing treatment models. They are dishonored by the professional practice of being satisfied with simple behavioral control over specific sexual patterns (sexual sobriety) as the primary objective of treatment.
Victims need recognition of the patterns of harm and abuse they experience and have endured, which goes way beyond the Pollyanna descriptions of “hurt and betrayal” caused by specific sexual acting out behaviors. Furthermore, female victims are violated further by being labeled “co-sex addicts” routinely by professionals and “educated that they have a disease of self perpetration” rather than being afforded therapeutic intervention for abuse and assessment and treatment for consequent acute and complex trauma (C-PTSD).
The Sex Addiction-Induced Trauma Model (SAITM) accounts for the clinical management and treatment of both sexual behaviors and SAIP. According to the model, sex addiction-compulsivity disorders are defined as “a complex system of sexual, personality and masculinity pathology, which may include the maintenance of a deceptive, compartmentalized sexual-relational reality, sexual-relational acting out behaviors, and other patterns of perpetration, abuse, and violation that causes serious PTSD and CPTSD (SAIT) in victims.”
The model proposes clinical management that includes assessing and diagnosing sex addiction-induced perpetrations and providing appropriate safety, stabilization, and clinical de-escalation for victims. Clinical management would also provide methodological treatment for perpetration-focused management, clinical resolution, and psychological integration. Clinical treatment would also include relational, family, and social considerations, as indicated, in a perpetration-victimization and post-traumatic clinical context and conscious framework.
The American Psychological Association’s Intimate Partner Abuse and Relationship Violence Working Group concluded, “We suggest that those involved in partner violence have specialized treatment needs and that those who treat them must do so with sensitivity and from a base of knowledge that comes from specialized training. Psychologists who do not have the requisite training potentially endanger their clients and are likely commit an ethical violation. Those who are teaching psychologists-to-be but who do not teach them about partner violence are abrogating their responsibility and risk perpetrating the conditions which foster this problem.”
Perpetration requires treatment and appropriate clinical intervention, not defensive denial, silence, and professional avoidance. Clinical pathology that contributes to serious harm and violation of others and human rights requires an organized clinical methodology and direct clinical management, not undefined, underdeveloped, or squeamish clinical approaches.
After all and in fact, it is these dynamics of sex addiction-induced perpetrations that often “induce trauma,” do more human damage, and accrue more human cost than sexual acting out behaviors alone ever possibly could.












